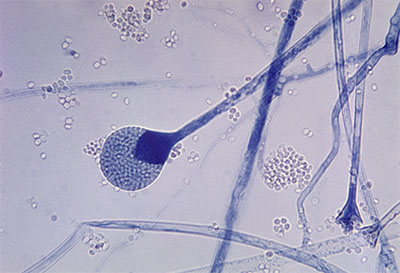
Mucormycosis is a devastating fungal disease caused by infection with pathogenic fungi from the taxonomic order Mucorales. The Mucor and Rhizopus genera are responsible for the majority of mucormycosis cases. Invasive mucormycosis occurs most often in patients with hematological malignancies undergoing chemotherapy, patients who have received hematopoietic stem cell (i.e. bone marrow) or solid organ transplants, and patients with diabetes mellitus. Mucormycosis can also present as rhino-orbital-cerebral mucormycosis (ROCM). ROCM has been closely associated with COVID-19 patients with diabetes mellitus, particularly patients in low- and middle-income countries.
Mucormycosis does not respond to the first-line anti-fungal drugs used to treat other invasive fungal diseases (such as invasive aspergillosis or invasive candidiasis), and delays in treatment increase the mortality rate from an already high 47% to 83%. Moreover, treatment for ROCM often includes highly invasive and life-altering (e.g. blinding) surgery. As a consequence, early diagnosis for both invasive mucormycosis and ROCM is critical for giving patients the best chance of survival and the highest possible subsequent quality of life.
Diagnostic challenges
Unlike other invasive fungal diseases such as invasive aspergillosis or histoplasmosis, no antigen-detection immunoassay for mucormycosis currently exists. Instead, diagnosis of mucormycosis is typically performed via fungal culture, histopathology, microscopy, or PCR using invasive biopsy specimens. Collecting these biopsy specimens (especially pulmonary specimens) has risks, particularly in the immunocompromised patients who are at the highest risk of contracting mucormycosis. In addition, fungal culture takes weeks for a result.
DxDiscovery solution
DxDiscovery is developing a lateral flow immunoassay (similar in format to the at-home COVID-19 test) for rapid (<20 min) and simple diagnosis of mucormycosis during early-stage infection. The assay is designed to be used with non-invasive or minimally-invasive specimens (e.g. urine, serum, or plasma) in order to reduce patient risk during specimen collection and to enable repeated testing for prospective monitoring of high-risk patients.
Market opportunity
The market for a mucormycosis diagnostic includes both symptomatic patient testing and prospective monitoring of particularly high-risk individuals. Among symptomatic patients, mucormycosis is diagnosed in 10-20% of patients where invasive aspergillosis is considered in a differential diagnosis. Importantly, the correct diagnosis (mucormycosis vs. invasive aspergillosis) is critical because the two fungal infections have very different treatments despite similar clinical presentations. As a consequence of the shared clinical presentation and shared profile of which patients are highest-risk, the clinical use and market size for the mucormycosis immunoassay with symptomatic patients would be similar to that of existing commercially successful immunoassays for diagnosis of invasive aspergillosis. Thus, the serviceable available market for testing of symptomatic patients is estimated to be approximately 200,000 tests per year in the United States alone.
Regarding prospective testing, approximately 200,000 individuals each year have health conditions that are known to increase their risk of developing mucormycosis (e.g. diabetic ketoacidosis, leukemia, neutropenia, or solid organ or hematopoietic stem cell transplantation). Diagnosing mucormycosis early in these high-risk patients would also be highly beneficial. Prospective monitoring of even just the 50,000 annual solid organ or hematopoietic stem cell transplant recipients in the U.S. twice-weekly for the first 12 weeks post-transplant would alone require 1.2 million tests per year.
Internationally, there are potentially hundreds of thousands of cases of ROCM annually. An affordable, rapid, point-of-care, lateral flow immunoassay that can be used even in clinics in resource-limited settings will be critical to reaching these patients.
R&D funding
DxDiscovery has been awarded a Small Business Innovation Research (SBIR) Phase I grant from the National Institute of Allergy and Infectious Diseases (NIAID) for development of the mucormycosis diagnostic.
For more information, please contact us: ContactUs@DxDiscovery.com